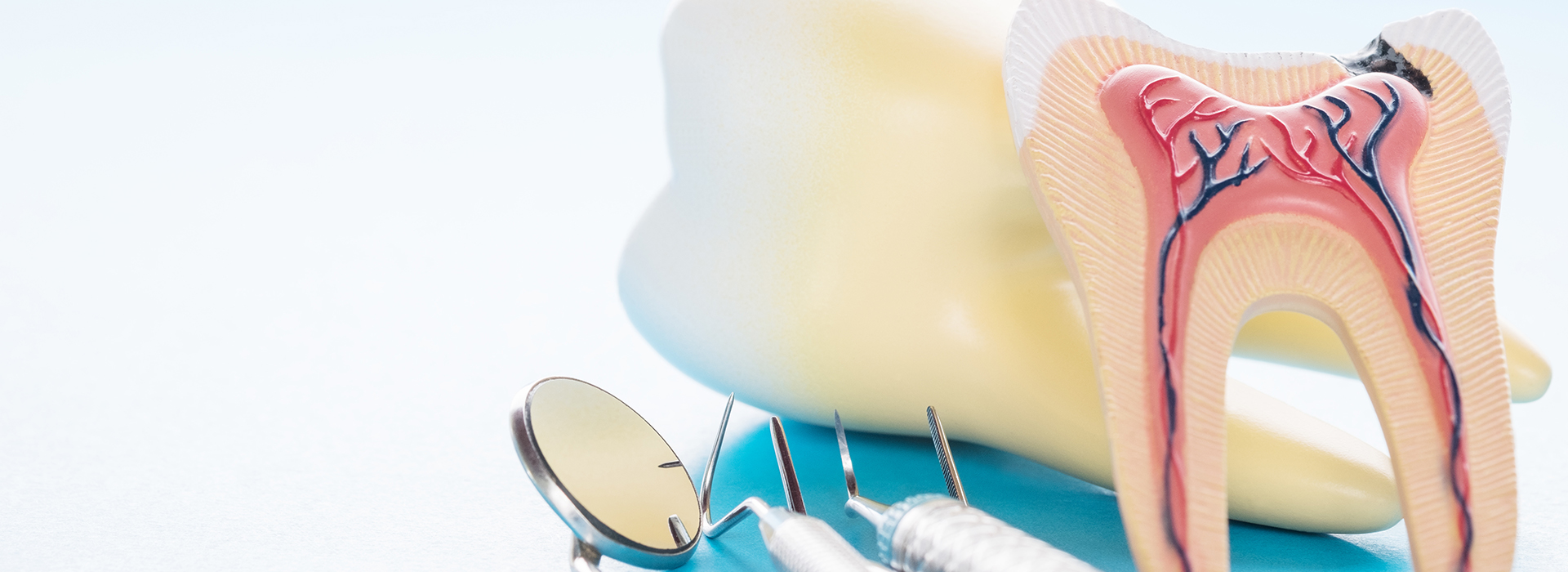
If a dental professional recommends root canal therapy for a troublesome tooth, try not to worry. Modern root canal treatment is a precise, predictable procedure designed to relieve pain, eliminate infection, and keep your natural tooth functioning in the long term. Compared with extraction and replacement, saving the tooth preserves chewing strength, maintains facial structure, and is often the gentlest route to restoring oral health.
At the office of Pearly Isles Dental, we combine modern instruments with a patient-centered approach to make treatment as comfortable and clear as possible. Our goal is to help you understand the reason for care, the steps involved, and what to expect during recovery so you can make a confident decision about your oral health.
Root canal therapy is focused on removing diseased or dead tissue from the inside of the tooth and sealing those spaces to prevent reinfection. When successful, this approach preserves the natural tooth root and crown, which supports efficient chewing and maintains the alignment of surrounding teeth. Preserving a natural tooth also avoids the additional procedures and maintenance sometimes required for dental implants or bridges.
Thanks to advances in techniques and biocompatible materials, root canal treatment now succeeds at very high rates in appropriate cases. The procedure can stop an active infection, relieve intense toothache, and restore stability to a tooth that would otherwise deteriorate. For many patients, a root canal is the most conservative option that protects both oral function and long-term dental health.
Beyond immediate relief, keeping the tooth helps preserve jawbone and soft tissue contours around the site. That anatomical preservation can make any future restorative work simpler and delivers a more natural result over time. Your dentist will weigh the condition of the tooth, surrounding bone, and overall health to recommend the most durable solution.

Each tooth has an inner chamber containing the dental pulp — a soft tissue made up of nerves, blood vessels, and connective tissue. While the pulp is essential during tooth development, a mature tooth can remain healthy after the pulp becomes inflamed, infected, or non-vital. When that happens, the tooth often begins to send warning signs that something is wrong.
Symptoms can vary. Some people experience sharp or throbbing pain that worsens with chewing or at night, while others may feel only occasional sensitivity to hot or cold. In other cases, the pulp may have been damaged for some time without obvious discomfort, and an issue is first detected during a routine exam or on an X-ray.
When the pulp tissue is irreversibly damaged, the risk of spreading infection increases and the tooth’s structure can weaken. Root canal therapy removes the compromised tissue, cleans and shapes the internal canals, and seals them so the tooth can be restored and preserved rather than removed.
Although symptoms vary, the following signs commonly indicate a tooth could benefit from root canal treatment:
Persistent discomfort that interferes with sleep, eating, or daily activity is a frequent sign of deep decay or pulp inflammation. Pain that intensifies with pressure or keeps returning should be evaluated promptly.
Teeth that react strongly to hot or cold and do not quickly return to normal after the stimulus is removed may have damaged pulp tissue that requires professional care.
Feeling pain from light pressure, such as when chewing or tapping the tooth, can indicate an irritated or infected nerve inside the tooth that should be assessed without delay.
A tooth that becomes noticeably darker than neighboring teeth may have experienced internal changes after trauma or chronic infection, which often accompany pulp damage.
Structural damage to a tooth can expose inner tissues to bacteria and trauma, increasing the likelihood that root canal therapy will be necessary to save the tooth.
Gum swelling or a small bump near the tooth can indicate an abscess or localized infection. These signs are reason enough to seek timely evaluation and treatment.
Advanced infection around the root can affect the supporting bone and connective tissues, producing mobility. Treating the infection and restoring the tooth structure often stabilizes the area.
Treating a problem before it becomes extensive typically leads to simpler care and a more predictable recovery. Some teeth develop internal changes or minor infections long before symptoms become severe; routine exams and X-rays can reveal these issues so they are addressed while the treatment remains straightforward.
Delaying care can allow infection to spread into surrounding bone or soft tissues, increasing the complexity of treatment and the risk of complications. Early intervention with root canal therapy often prevents those downstream problems and preserves more of the natural tooth structure.
Your dentist will consider the condition of the tooth, the health of nearby tissues, and your medical history when recommending treatment timing. When root canal therapy is advised, scheduling it within a reasonable timeframe helps protect overall oral health and reduces the chance of emergency situations.
Root canal therapy today uses precise instruments and advanced cleaning methods to treat the internal portion of the tooth. After numbing the area, the clinician gains access to the pulp chamber, removes the diseased tissue, and carefully shapes and irrigates the canals to eliminate bacteria and debris.
Some teeth can be treated in a single appointment; others require two or three visits depending on complexity, the number of canals, and whether an active infection needs additional management. Once the internal spaces are prepared, they are filled with a biocompatible material and sealed to prevent reinfection.
Local anesthesia usually provides comfortable care, and for patients who feel anxious, mild sedation options are available to make the experience more relaxed. After the internal work is complete, the tooth typically requires a protective restoration — often a crown — to restore strength and function for years to come.
At Pearly Isles Dental, patient comfort and clear follow-up instructions are essential parts of care. After treatment, most people experience mild soreness that fades within a few days. Your dentist will explain what to expect, how to manage any discomfort, and when to resume normal activities.
Initially, you may notice temporary numbness until the local anesthetic wears off — avoid chewing until normal sensation returns to prevent accidental injury. If antibiotics or pain medication are prescribed, follow the instructions carefully and finish the course as directed.
A tooth that has undergone root canal therapy is more brittle until it receives a permanent restoration. Chew with care on the opposite side and avoid hard or sticky foods until a crown or other definitive restoration is placed. Maintaining excellent oral hygiene and attending regular dental visits will help the treated tooth remain healthy for many years.
Numbness and mild tenderness are expected right after treatment. These sensations typically resolve quickly, but follow any specific aftercare steps your dentist provides.
You may feel slight soreness for several days; over-the-counter pain relievers are often sufficient. If pain worsens or persists beyond the expected timeframe, contact the office for evaluation.
If antibiotics are prescribed to control infection, complete the entire course as instructed, even if symptoms improve before the medication is finished.
A temporary filling protects the treated area but doesn’t fully restore strength. Avoid chewing on the treated tooth until your permanent restoration is placed.
Continue brushing and flossing gently around the treated tooth to support healing and prevent new problems from developing.
Placing the crown or definitive restoration in a timely manner restores function and helps prevent fracture of the remaining tooth structure.
With careful treatment and routine care, a tooth that has had root canal therapy can remain healthy and functional for many years — often a lifetime. If you have questions about symptoms you’re experiencing or want to learn whether root canal therapy is appropriate for a particular tooth, please contact us for more information.
Root canal therapy treats the inner portion of a tooth when the dental pulp becomes inflamed, infected, or non‑vital. The procedure removes diseased tissue, cleans and shapes the internal canals, and seals the spaces to prevent reinfection. Treating the tooth in this way preserves the natural root and crown instead of removing the tooth.
Preserving a natural tooth helps maintain chewing efficiency, the alignment of adjacent teeth, and the facial contours that rely on tooth roots and jawbone. When a tooth can be saved rather than extracted, patients often avoid more extensive restorative work and maintain better long‑term oral function. Your dentist will evaluate the tooth and recommend root canal therapy when it offers the most predictable path to lasting oral health.
Common signs that a tooth may need root canal therapy include persistent or worsening tooth pain, pronounced sensitivity to hot or cold that lingers, and discomfort when biting or tapping the tooth. Other warning signs include visible darkening of the tooth, gum swelling or a small bump near the tooth, and loosening or mobility of the affected tooth. These symptoms often indicate pulp damage or infection that should be assessed promptly.
Some teeth develop internal problems without obvious pain, so routine exams and X‑rays play an important role in detecting issues early. If you notice any of the signs above or have had dental trauma, schedule an evaluation so the condition can be diagnosed and treated before it progresses. Early assessment typically leads to simpler treatment and a more predictable outcome.
Root canal therapy begins with numbing the area using local anesthesia to ensure patient comfort during the procedure. The clinician creates a small access opening in the crown, removes the infected or damaged pulp tissue, and carefully cleans and shapes the internal canals using specialized instruments and disinfecting solutions. Once the canals are prepared, they are filled with a biocompatible material and sealed to prevent reinfection.
Some teeth can be treated in a single visit while others require two or more appointments depending on complexity and the presence of active infection. A temporary restoration protects the tooth until a definitive restoration is placed, and the dentist will discuss the timing and type of final restoration needed to restore strength and function. The overall goal is to eliminate infection while preserving as much of the natural tooth as possible.
Modern root canal treatment is designed to be comfortable and is performed under effective local anesthesia so most patients do not experience pain during the procedure. In many cases the treatment relieves the severe toothache that prompted the visit, because the source of the pain is removed when the infected tissue is cleaned out. For patients who feel anxious or require additional comfort, mild sedation options are available to help relax during care.
After the procedure it is common to feel mild soreness or tenderness for a few days as surrounding tissues heal, and over‑the‑counter pain relievers typically manage this discomfort. If pain increases, swelling develops, or symptoms persist beyond the expected recovery period, contact the office for evaluation. At Pearly Isles Dental we emphasize comfort and clear aftercare instructions so patients understand what to expect and how to manage post‑treatment sensations.
Recovery after a root canal is generally brief; most people return to normal activities within a day or two while mild soreness subsides over several days. You may experience temporary numbness until the local anesthetic wears off and should avoid chewing on the treated tooth until sensation returns to prevent accidental injury. If antibiotics or pain medication are prescribed, follow the directions carefully and complete the course as recommended.
The treated tooth remains more brittle until it receives a permanent restoration, so avoiding hard or sticky foods is important until a crown or other definitive restoration is placed. Your dentist will schedule a follow‑up to monitor healing and plan the final restoration that restores full function and protection. Prompt placement of the permanent restoration helps ensure the long‑term success of the treated tooth.
Many teeth that receive root canal therapy, especially molars and premolars, benefit from a crown or similar protective restoration to restore strength and prevent fracture. The internal cleaning process can leave the remaining tooth structure more brittle, and a crown helps distribute chewing forces and seal the tooth against new bacterial invasion. Your dentist will evaluate the amount of remaining tooth and recommend the most appropriate restoration type.
In some cases a direct buildup or onlay may be sufficient for teeth with minimal structural loss, while heavily restored or weakened teeth usually require full coverage. Timely placement of the final restoration is an important step in preserving the tooth long term and reducing the chance of future complications. Discuss restoration options with your dentist so you understand the recommended timeline and materials for your situation.
Maintaining good oral hygiene is essential after root canal therapy; continue regular brushing and flossing to prevent new decay and protect surrounding teeth and gums. Avoid chewing on the treated tooth until the permanent restoration is in place, and be mindful of hard or sticky foods that can damage the temporary filling or the remaining tooth structure. If you grind your teeth or clench, discuss protective options such as a night guard to reduce the risk of fracture.
Attend follow‑up appointments as recommended so the dentist can place the final restoration and monitor healing. If you notice new pain, swelling, or drainage around the treated tooth, contact the office promptly for evaluation. Long‑term success depends on both high‑quality treatment and consistent home care and professional maintenance.
Root canal therapy is highly successful in appropriate cases, but failure can occur when anatomy is complex, canals are missed, a tooth fractures, or reinfection develops. If symptoms recur or radiographs show persistent problems, retreatment of the canals or endodontic surgery (such as an apicoectomy) are common options to address residual infection while preserving the tooth. Your dentist or an endodontist will review the cause and recommend the most suitable next steps.
When retreatment or surgery is not feasible or does not resolve the issue, extraction followed by a dental implant or bridge becomes an alternative to restore function and appearance. The decision between retreatment and replacement depends on the tooth’s restorability, patient health, and long‑term prognosis. A timely evaluation and clear explanation of options help patients choose the approach that best fits their needs.
Root canal therapy removes infected tissue and seals the tooth to prevent the spread of bacteria, which can protect both oral and systemic health. Modern endodontic materials are biocompatible, and treating an active dental infection reduces the risk of more serious complications that can arise when oral infections go untreated. The procedure is performed with sterile technique and careful diagnosis to maximize safety and effectiveness.
If you have a medical condition such as a weakened immune system, certain heart conditions, or take medications that affect healing, inform your dental team so they can coordinate care with your physician if needed. In selected cases antibiotics or specific precautions may be advised to manage risk. Overall, root canal therapy is a standard, safe treatment when performed by trained clinicians and followed by appropriate restorative care.
Before your appointment, gather a list of current medications, medical conditions, and any recent changes to your health to share with the dental team. If you plan to use sedation or feel anxious, arrange for a companion to drive you home and follow any pre‑procedure instructions about eating or drinking provided by the office. Be prepared to ask questions about the procedure, expected steps, and the timeline for the final restoration so you feel informed and confident.
On the day of treatment arrive with comfortable clothing and allow time to complete any necessary paperwork or X‑rays. The clinician will review your medical history, explain anesthesia and sedation options if applicable, and outline post‑treatment care tailored to your situation. At Pearly Isles Dental we focus on clear communication and patient comfort to help you prepare for a smooth and predictable experience.
